By Lyra Fontaine
ME researchers developed a device that could measure brain pressure to better understand sleep issues or traumatic brain injury.
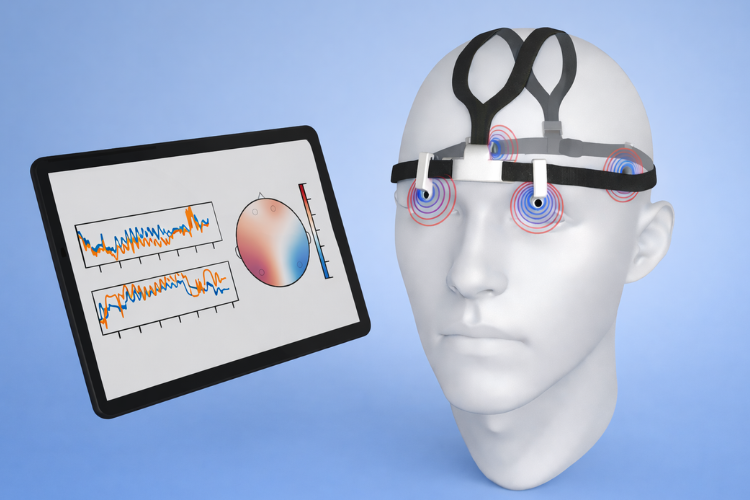
Graphic of the wearable device, with the circles representing the areas where brain pressure is measured through tiny electric fields. Photo provided by Sanggyeun Ahn.
The pressure in our brains changes based on time of day, the activity we’re doing and when an injury occurs. Researchers in ME Professor Jae-Hyun Chung’s lab have developed a non-invasive, wearable device that can measure brain pressure, which shows promise in helping to diagnose brain injury and sleep disorders.
“Our device is innovative because it can continuously monitor brain pressure in multiple locations,” says Chung. “We found that we can potentially use brain pressure to measure traumatic brain injury and chronic sleep disorder.”

Graduate students Shawn Kim and Changwoo Lee are checking a sleep mask. Photo provided by Changwoo Lee.
The device is the first that can monitor brain pressure for more than 20 hours non-invasively. While typically brain pressure is measured by surgically inserting a catheter or sensor into the brain, this device is non-invasive and easy to use, which could make brain health monitoring more accessible. The researchers collaborated with the UW Medicine Department of Emergency Medicine and Department of Cardiology, and Dongguk University Ilsan Korean Medicine Hospital in South Korea.
The wearable device’s capacitive sensors are made of carbon-nanotube paper composite electrodes. These sensors detect brain pressure changes in different areas through electric field variations caused by blood vessel pulsations, brain fluid changes, and tissue vibrations.
The researchers were their own first test subjects. They found that pressure varies in parts of the brain throughout the day, influenced by factors including sleep, body position, breathing patterns, eating and drinking, cognitive activity like solving math problems, and physical exertion such as climbing stairs.
“That’s how we found the initial evidence to pursue this idea,” says Ph.D. student Shawn Kim. “The first test I did was changing my body posture by going from laying down to sitting up, positions that are known to change brain pressure.”
Measuring sleep quality

Sleep mask monitoring local brain pressure changes near eyes. Photo provided by Changwoo Lee.
We know we need sleep to benefit our health, but assessing chronic sleep problems, such as insomnia or chronic sleep deprivation, can be a challenge. There’s a lack of objective monitoring methods, the researchers say.
Current sleep studies that measure brain waves, eye movement, heart rate and more can be expensive and time-consuming. A wearable device could be a simpler, lower-cost alternative. Current home-based tests are primarily based on electrical signals and respiratory events, which doesn’t provide a full picture of sleep behavior, Chung says.
The researchers found that brain pressure distribution was one key way to determine sleep deficiency, with brain asymmetry indicating higher-quality sleep. They also found that more frequent fluctuations in brain pressure were linked to worse perceived restfulness.
The researchers embedded a cloth sleep mask with nanostructured capacitive sensors to monitor brain pressure and eye movement during sleep. Since brain pressure fluctuates with circadian rhythms, sleep stages and events like sleep apnea or rapid eye movement, it could be a way to assess sleep quality.
In addition, the researchers worked with collaborators at Dongguk University Ilsan Korean Medicine Hospital on a nap study. Forty volunteers wore the device while napping and then rated their sleep quality. A machine learning analysis of the study found correlations between brain pressure patterns and chronic sleep problems. One notable finding: sleep apnea was associated with elevated brain pressure in a particular area of the brain.
“We hypothesized that good and bad sleep would show a difference in brain pressure in our sensor readings,” says Ph.D. student Changwoo Lee. “We tested 20 self-described good sleepers and 20 self-described bad sleepers and saw our hypothesis worked.”
The technology could be used as a tool to detect subtle brain activities in response to various stimulations, similar to functional brain MRI, says Younghoon Kwon, a professor in the UW Medicine Division of Cardiology, who contributed to the research.
“While a work in progress, this novel technology gives us a glimpse into what the future ‘functional’ brain monitoring may look like in various settings,” Kwon says.
Sensing brain injury
Traumatic brain injury (TBI), brain damage caused by an outside force, is a common cause of disability and death in adults, according to UW Medicine. No standard tool exists to monitor TBI without invasive procedures, Chung says. While currently used tools measure blood flow or neuron activity, the researchers are trying to understand brain activity through measuring brain pressure at different sites.
Brain pressure is a promising way to assess trauma in brain injury, Chung says. Medical providers might image the brain to determine the severity of the TBI and whether urgent surgery is needed. However, currently used and clinically validated imaging tools and tests don’t always identify damage from mild TBIs, according to the National Institutes of Health.
Providers typically monitor patients for several hours, but wearable devices like the one Chung’s lab developed could be a way to continuously monitor brain pressure to make sure people experiencing TBIs are treated in time. The researchers found that brain pressure changed during and after injury.
Kim was part of the team that researched and wrote a paper on how brain pressure sensing could help monitor TBI. The team conducted experiments, collaborated with UW Medicine to test sensors, and used statistical and machine learning approaches.
“The way we are looking at the brain is not something people have thought of before,” Kim says. “Because our method of electric sensing is different from previous methods, we’re able to extract a novel signal and get data that people have not seen before to potentially improve the way brain injuries are monitored.”
This technology could make brain pressure monitoring accessible beyond critical care environments, according to Nathan White, professor at the UW Medicine Department of Emergency Medicine, who contributed to the research.
The researchers are planning a future clinical study that focuses on how brain pressure can help measure the severity of TBIs, and a study about how sleep apnea relates to increased brain pressure.
Originally published May 11, 2026