By Chelsea Yates
In this story, we highlight six research projects led by ME faculty, each committed to advancing cardiovascular health and saving lives.

Heart disease is the leading cause of death for adults in the U.S. According to the Centers for Disease Control and Prevention (CDC), about 610,000 people die of heart disease every year — that means it is the cause of 1 in 4 deaths. The CDC also estimates that 735,000 Americans experience a heart attack each year, and nearly 30% of those are repeated occurrences.
UW mechanical engineers have long been committed to advancing health technologies. Several researchers are enabling health care providers to better understand and treat cardiovascular disease, including heart attack, stroke, arrhythmia, congestive heart failure, angina and more.
Here we highlight six research projects currently underway by ME faculty, each committed to accelerating engineering and saving lives:
Clearing clogged arteries
By innovating endoscope technology, ME research professor Eric Seibel is working to create safer and more effective therapies that open blockages in the cardiovascular system. Endoscopes are generally used to look inside the body, but Seibel is exploring ways to enhance a scanning fiber endoscope (SFE) invented at UW in the early 2000s so that it can deliver laser light for multiple purposes. This would allow the endoscope to image, diagnose and remove arterial fatty plaque and fibrous clots. Currently, no other scope can look down these vessels in resolutions as high as the SFE does. And because it is flexible and small (1-mm diameter), it’s an excellent candidate to become the first high-resolution catheter scope, or “eye” at the tip of a guidewire used in the cardiovascular system.
Seibel has been working closely with UW Medicine’s Center for Cardiovascular Innovation and the Puget Sound-based startup company VerAvanti (NIH Small Business Innovation Research program) to manufacture and make this device more widely available so that cardiologists, surgeons and other health care professionals can better diagnose and treat individuals who are at risk for stroke and/or heart attacks.
Designing better hearts for children
Children born with congenital heart defects — such as narrowed or closed valves, poor connections among blood vessels, and problems affecting the heart’s chambers or muscle — often must undergo several surgeries to rebuild their hearts. Currently, surgeons build patches of graft tissue to reshape the arteries and chambers as needed on the spot in the operating room. ME associate professor Alberto Aliseda wants to make this process more efficient. He is working with pediatric cardiologists and surgeons to develop tools and processes to create these patches before surgery, thereby minimizing the time that a young patient’s heart is stopped during the operation.
Aliseda’s research team hopes to create physical models so surgeons can practice and achieve better results, and researchers can measure the flow velocity, pressure and energy more accurately to improve calculations and optimization.
Stronger hearts
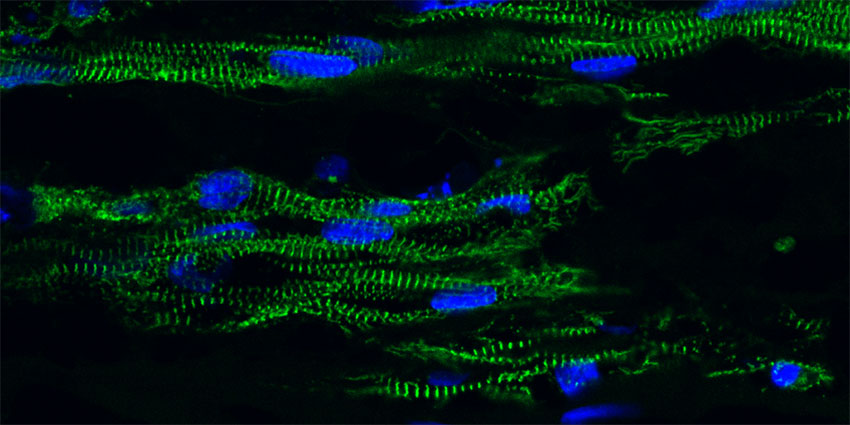 Heart muscle cells made from stem cells and grown in a 3-D tissue construct.
Heart muscle cells made from stem cells and grown in a 3-D tissue construct.
ME associate professor Nathan Sniadecki is developing new engineering approaches to unlock the potential of stem cell-derived cardiomyocytes, or cardiac muscle cells. These can be used as a source of new heart muscle cells for scientific efforts ranging from regenerative medicine to pharmacology studies to heart disease research. Sniadecki has innovated new tools and methods to measure the functional performance of stem cell-derived cardiomyocytes at the single cell and at the tissue level.

Engineered heart tissue made from stem cells is suspended between two flexible, silicone pillars to measure their contractile strength.
Recently, his lab has developed a tissue-engineered approach to grow cardiomyocytes in a 3D construct that beats like heart tissue and responds to pharmacological treatments and mechanical cues. This “heart-in-a-dish” platform measures the contractile force of the tissue and is used to examine new techniques to mature the cells, screen new pharmacological treatments for heart disease, or study inherited forms of heart muscle disease.
Improving LVAD placement and management
An individual with advanced heart failure whose heart is no longer able to pump enough blood to meet his body’s needs may be recommended for left ventricular assist device (LVAD) implant surgery. LVADs are surgically implanted devices that attach to the heart to help it pump more blood with less work.
ME associate professor Alberto Aliseda is working to improve the implantation process and management post-surgery by applying computational fluid dynamics, 3D printing and design optimization to the surgical procedures and the clinical decisions regarding patients’ pumps. By identifying the best location to implant the LVAD and better managing its performance, this work will help reduce stress levels on the blood and cardiac tissue, help doctors provide more individualized care to patients, and help researchers better understand complications surrounding advanced heart failure.
Unlocking the secrets of heartbeats
Implantable Cardioverter Defibrillators (ICDs) can prevent sudden death in patients with congestive heart failure. An ICD is a battery-powered device placed under the skin to monitor heart rate. It is connected to the heart by thin wires; if ventricular fibrillation (VF) or a sudden death is detected, the device delivers a powerful electric shock to restore a normal heartbeat.
While this device can extend a patient’s life, there is currently no way of knowing when he or she might experience an abnormal heartbeat and thus receive a jolting shock. ME professors Per Reinhall and Steve Brunton are exploring how to use machine learning to detect signs of irregularities in the heart rate data of patients with ICDs before the onset of VF. By reviewing and assessing the ECG data from 1,000 heart failure patients with ICDs, they hope to identify patterns that will predict when a shock might occur and provide patients with advanced warning so that they may prepare accordingly.
Engineering heart tissue with optical tweezers
 Optical tweezers manipulate cells. See related video on YouTube.
Optical tweezers manipulate cells. See related video on YouTube.
ME and ISE assistant professor Ashis Banerjee is investigating how to develop better-engineered heart tissue using optical tweezers as a complementary technique to micro-molding or bioprinting. Optical tweezers use a highly focused laser beam to manipulate microscopic objects in three dimensions; Banerjee’s team is exploring how to use them to precisely position endothelial cells on top of growing cardiomyocytes. He hopes doing so will allow his team to hierarchically assemble entire heart tissue structures artificially in vitro, leading to more efficient and reliable methods of creating better performing heart tissue overall.
Learn more about ME’s innovations in health technology.
Originally published March 26, 2018
